Background
Nearly 25% of cancer patients harbor clonal hematopoiesis of indeterminate potential (CHIP). Detection of clonal hematopoiesis (CH) in routine clinical practice is increasing due to incidental findings during sequencing analysis of circulating cell-free DNA (cfDNA) or exploration of unexplained cytopenia. To improve clinical management of these patients in our institution, we set up a multidisciplinary molecular tumor board (MTB) dedicated to patient cases with CH, CHIP, and clonal cytopenia of undetermined significance (CCUS) in 2022.
Methods
Between June 2022 and June 2023, our MTB reviewed a total of 345 cases, of which 212 referred by the solid tumor MTB and 133 referred by hematologists. The former 212 cases with CH were identified through cfDNA sequencing (FoundationOne Liquid CDx) within the Gustave Roussy Cancer Profiling study (NCT04932525), which includes some genes recurrently mutated in hematologic malignancies ( ASXL1, DNMT3A, IDH1, IDH2, JAK2, MPL, MYD88, SF3B1, TET2, U2AF1). A variant allele frequency (VAF) of at least 10% for the CH mutation was required to refer cases to the MTB, except for JAK2, MPL, and MYD88 mutations. The latter 133 cases were screened for CH mutations on peripheral blood leukocytes using a next-generation sequencing (NGS) assay targeting 174 genes recurrently mutated in hematologic malignancies. In addition to molecular data, standard clinical and biological parameters were recorded for each individual case.
Results
Patients referred by the solid tumor MTB
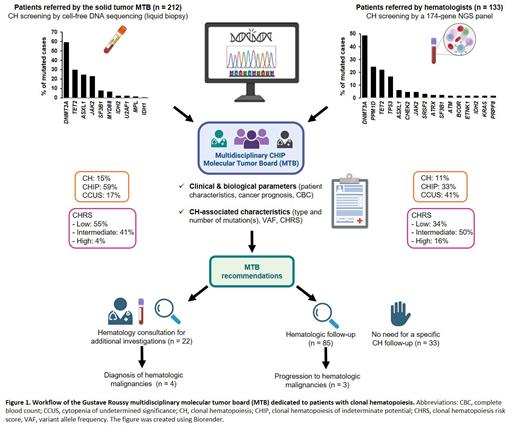
In this cohort of 212 patients, median age was 72 years old (range, 48-91), sex ratio (M/F) was 1.4, median prior anticancer treatment lines was 2 (0-9), and time between MTB and cancer diagnosis was 2.3 years (0.2-34). The most frequent tumor types were lung (23%), colorectal (20%), prostate (19%), gynecological (12%) and breast (9%) cancers. The most frequently mutated genes were DNMT3A (59%), TET2 (30%), ASXL1 (24.5%), JAK2 (23%), SF3B1 (7.5%), and MYD88 (6%), with a median VAF of 4.2%, 3.0%, 8.5%, 1.0%, 5.0%, and 0.20%, respectively. Fifty percent of patients harbored more than 1 mutation. Six patients had a known history of myeloproliferative neoplasm (MPN). The proportion of cases with CH, CHIP, and CCUS was 15%, 59%, and 17%, respectively. The CH risk score of myeloid malignancy (CHRS, Weeks et al.) could be calculated in 126 cases but may underestimate risk due to the limited gene list considered, and revealed 69 (55%) low-risk, 52 (41%) intermediate-risk, and 5 (4%) high-risk patients. Our MTB recommended hematologic consultation for additional investigations in 58 patients, of which 22 were actually referred (main reason for not referring patients was advanced cancer disease). Four patients were diagnosed with hematologic malignancy (1 MPN, 1 chronic myeloid leukemia, 2 myelodysplastic syndromes [MDS]).
Patients referred by a hematologist
In this cohort of 133 patients, median age was 69 years old (53-89), and sex ratio (M/F) was 0.6. Eighty-six percent of patients had a cancer history, median prior anticancer treatment lines was 2 (0-7), time between MTB and cancer diagnosis was 3.5 years (0.2-34). The most frequent tumor types were lymphoid disorders (39%), breast cancer (15%), and gynecological cancer (15%). The proportion of CH, CHIP, and CCUS was 11%, 33%, and 41%, respectively. The most frequently mutated genes were DNMT3A (48,5%), PPM1D (24%), TET2 (22%), TP53 (17%), ASXL1 (6%), JAK2 (4.5%) and CHEK2 (4.5%), with a VAF of 2.5%, 2,3%, 4.0%, 2.0%, 8.0%, 1.0%, and 2.5%, respectively. Sixty percent of patients harbored more than 1 mutation. The CHRS could be calculated in 98 cases and revealed 34% low-risk, 50% intermediate-risk, and 16% high-risk CH patients. No need for a specific follow-up was recommended by the MTB in 33 patients. Among the 85 patients with hematologic follow-up, 3 (for which the CHRS was intermediate in 2 cases and high in 1 at the time of MTB evaluation) rapidly progressed to a myeloid malignancy ( Figure 1) (2 MDS and 1 MDS/MPN).
Conclusions
Our study highlights the utility of a MTB dedicated to CH, CHIP and CCUS for the identification of high-risk patients, early detection of hematologic malignancies, and appropriate therapeutic management. Long-term follow-up is needed to validate the CHRS but the design of a specific score for patients with cancer may be helpful due to the specific features of this population (high prevalence of PPM1D mutations, post-treatment cytopenia).
Disclosures
Micol:Servier: Honoraria; JazzPharmaceuticals: Honoraria; Gilead: Honoraria; Abbvie: Honoraria. Aldea:Sandoz: Research Funding; Viatris: Honoraria. Castilla-Llorente:Gilead/Kite: Consultancy, Other: Travel support; Nektar Therapeutics: Consultancy. De Botton:Astellas Pharma a/s Nordic Operations: Honoraria; Abbvie: Honoraria; Celgene: Honoraria; Jazz Pharmaceuticals: Honoraria; FORMA Therapeutics: Research Funding; Novartis: Honoraria; Pfizer: Honoraria; Agios: Research Funding. Bernard:PFIZER: Speakers Bureau. Italiano:AstraZeneca: Honoraria; Bayer: Honoraria; Deciphera: Honoraria; Daiichi Sanky: Honoraria; Novartis Roche: Honoraria; AstraZeneca: Research Funding; Bayer: Research Funding; BMS: Research Funding; Merck: Research Funding; MSD: Research Funding; Pharmamar: Research Funding; Roche: Research Funding.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal